Breast cancer is the most common type of cancer among American women. Experts estimate that of the women who live to be 85, one in nine will get the disease at some point in her life. In fact, each year more than 184,000 women are diagnosed with breast cancer--that's equivalent to a woman learning she has it about every three minutes--and over 44,000 women die annually of the disease. Only lung cancer causes more cancer deaths among women.
Who's At Risk?
The greatest risk factor for developing breast cancer is being female. A prior history of the disease increases the risk as well. Here are some other factors associated with an increased risk.- Age. About 75 percent of all breast cancers are found in women over the age of 50. The disease is uncommon in women under the age of 35 and quite rare in women under the age of 25.
- Family History. Risk increases if a woman has a mother or sister who has had breast cancer before menopause.
- Early Menstruation. A woman whose first menstrual period was before the age of 12 is at higher risk.
- Late Menopause. Having started menopause after the age of 55.
- Delayed Childbearing. Never having had a child or having the first child after the age of 30.
- Diet. A diet high in fat has long been thought to increase the risk of breast cancer. A recent Harvard study disputes that belief, however. Researchers there reviewed studies involving a combined total of nearly 338,000 women and found that even extremely low fat diets (less than 20 percent of calories from fat) failed to reduce breast cancer risk. Research into any connection between dietary fat and breast cancer continues. Meanwhile, remember that eating less saturated fat significantly cuts the risk of heart disease, which kills more women than breast cancer does.
- Smoking. Recently, an American Cancer Society (ACS) study found that while smoking may not cause breast cancer, it does seem to increase a woman's chance of dying from the disease by 25 percent.
What Are The Signs?
You should see your doctor if you notice any of the following changes in your breasts:- A lump in the breast or under the arm.
- A change in the normal size or shape of your breast.
- Spontaneous discharge coming out of your nipple.
- A change in the color or feel of the skin of the breast or areola.
- A sudden onset of pain in the breast.
What Is The Best Defense Against Breast Cancer?
Early detection. To ensure the widest range of treatment options, it is important to detect breast cancer as early as possible. With prompt treatment, the outlook for a cure is good. According to the National Cancer Institute (NCI), the five-year survival rate for women whose tumors haven't spread beyond the breast is 92 percent. When the cancer has spread to nearby lymph nodes under the arm, the rate decreases to 71 percent, dropping drastically to 18 percent once the cancer has spread to the liver, lungs or brain.Detecting Breast Cancer
There are three main ways women should screen for breast cancer:- Breast Self-Examination. Women's breasts come in many sizes and shapes. Age, menstruation, pregnancy, menopause and taking birth control pills or other hormones can all cause breast changes. It is important to learn what is normal for you. This can be done by regularly examining your breasts. A breast self-examination (BSE) is easy to do and a good way to take charge of your health.
Beginning at age 25, women should do a BSE regularly after menses. Being familiar with the usual appearance and feel of your breasts will make it easier to notice any changes from month to month. If you discover any of the symptoms listed above, see your doctor as soon as possible. (See the step-by-step guide to BSE.)
- Physical Breast Exam. Periodic breast examination, or palpation, by a health professional is an important step in early detection. During the exam, the doctor feels the breast and underarm with his or her fingers, checking for lumps. All women should have breast examinations as part of their routine checkups. Women 30 and older should have them annually.
- Mammography. A mammogram is an x-ray of the breast. It can reveal tumors and other changes in the breast too small to be felt by hand. When high-quality equipment is used and the x-rays are read by well-trained radiologists, 85 to 90 percent of cancers are detectable. Of the 10 to 15 percent of cases that don't show up on mammograms, most occur in younger women since they have denser, more fibrous breast tissue.
How a mammogram works: The breast is placed between two plates and pressure is applied to ensure a clear picture. That pressure may be uncomfortable, but the test only lasts a few minutes. Two x-rays are taken of each breast, one from the top and one from the side. Although some women are concerned about the risk of cancer posed by radiation during mammography, the actual risk is very small.
Especially good news for women with dense breasts: there are two new detection methods that make it easier to pick up tumors that are hard to spot on mammograms. Ultrasound offers a non-invasive way of viewing tissue using ultra-high-speed sound waves. Miraluma scintimmagraphy involves an intravenous injection of a radioactive dye. The isotope is absorbed by breast cancers and the areas then show up on photos taken with a special camera.
How Is Breast Cancer Diagnosed?
A biopsy is the only sure way to know whether a breast lump or a suspicious area seen on a mammogram is, in fact, cancer. A biopsy is a microscopic analysis of cells taken from the lump to determine if they are cancerous. The cells can be obtained by fine-needle aspiration, in which a few cells are extracted using a thin needle and a syringe, or by open biopsy, in which a larger sample of tissue is surgically removed.The good news: Four out of five breast lumps are not cancerous. Often the lump is a fluid-filled cyst, which can be drained through needle aspiration or diagnosed by ultrasound. If the lump is a solid tumor, a biopsy should be performed for tissue analysis. Frequently, the lump is removed at the time of biopsy. If the lump is left in place, a tissue diagnosis should be obtained by fine-needle aspiration or core needle biopsy, in which a larger tissue sample is drawn out. The lump should then be checked regularly for changes.
What Are The Treatment Options?
The choice of treatment for breast cancer depends on the stage of the cancer (whether it has spread to other places), the type of breast cancer, and certain characteristics of the cancer cells (such as how fast they are growing). The woman's age, whether she has had menopause and her general health, also help the doctor develop a treatment plan that best fits the woman's individual circumstances and values. A woman might want a second doctor to review her diagnosis and treatment plan. A short delay in beginning treatment should not reduce the chances of its success.The treatment options for breast cancer are surgery, radiation therapy, chemotherapy and hormone therapy. The doctor may recommend just one method or a combination, depending on the patient's needs. In some cases, a woman may be referred to other doctors for different therapies, such as oncologists for chemotherapy.
- Surgery. There are several different types of surgery for breast cancer. Here are some of the options:
Breast conserving surgery (lumpectomy, partial mastectomy, quadrantectomy) removes just the cancerous lump with some surrounding healthy breast tissue and usually some lymph nodes from under the arm. About two to three weeks after surgery, patients begin radiation therapy, which generally consists of a five-day-a-week regimen for six weeks. Research has shown that when combined with radiation, lumpectomy is as effective as mastectomy in treating early stage breast cancer and is preferable since a women retains her breast.
Sentinel node biopsy, a new procedure for testing the lymph nodes of women with early-stage breast cancer, is sparing women form having unaffected lymph nodes removed. Sentinel nodes are found under the arm near the breast and ar the first ones into which a tumor will drain. Researchers have found that if the sentinel nodes are free of cancer, the disease has not spread to the rest and no more nodes need to be removed. If a sentinel node is cancerous, however, more nodes must be removed.
Modified radical mastectomy removes the breast, the lymph nodes under the arm and the lining over the chest muscles (leaving the muscles intact). This procedure is an alternative to breast conserving surgery and radiation therapy. Due to long held beliefs by physicians and patients, this remains the most common type of surgery for breast cancer.
Total or simple mastectomy removes the breast and the lining over the chest muscle below the tumor. It is used to treat extensive ductal carcinoma in situ (abnormal cells found in the milk duct). Though controversial, it is also sometimes performed to prevent breast cancer in women at inordinately high risk of developing the disease due to a defective gene, which may account for about five percent of all breast cancers.
- Adjuvant Therapy. A doctor may advise a woman with early stage breast cancer to supplement surgery with another form of therapy. Called adjuvant therapy, this added regimen can help prevent cancer from recurring by killing cancer cells that may still be lingering in the body undetected.
Radiation Therapy (or radiotherapy) uses high-powered rays to damage cancer cells and stop them from growing. Radiation may come from an x-ray machine outside the body (external radiation) or from radioactive materials placed directly in the breast through thin plastic tubes (implant radiation). Sometimes both are used. Radiation is usually used after a lumpectomy to make sure any cancer cells in the remaining breast tissue is destroyed.
Chemotherapy uses drugs to kill cancer cells. These drugs may be taken orally or injected into a muscle or vein. Chemotherapy is administered in cycles--a treatment period followed by a rest period, then more treatments, and so on. Although it depends on the type of drugs used, chemotherapy generally does not require a hospital stay. Chemotherapy is usually used after a mastectomy if there are signs that the cancer has spread beyond the breast.
Hormone Therapy keeps cancer cells from getting the hormones they need to grow. If tests show the cancer is receptive to hormones, drugs may be administered to alter the way the hormones work or surgery may be performed to remove organs (such as the ovaries) that manufacture the offending hormones.
- Future Forecast. Research into the best ways to eradicate breast cancer and keep it from coming back continue. Two recent findings seem promising:
Combination Therapy. Two studies have shown that combining chemotherapy and radiation dramatically increases the survival rates among women who have had mastectomies. The first study, from Denmark, found that cancer grew back in only 9 percent of women treated with both therapies compared to 32 percent of women treated with chemotherapy alone. The other study, from Canada and published in the New England Journal of Medicine, reported equally impressive results: After 15 years combination therapy patients had 33 percent less chance of the cancer coming back and 29 percent less chance of dying from breast cancer.
Pre-operative Chemotherapy. A large study by the National Surgical Adjuvant Breast and Bowel Project (NSABP) has found that in some cases giving chemotherapy before surgery can reduce the size of a tumor enough to allow a woman to have a breast-saving lumpectomy instead of a mastectomy. The new findings apply to the 5 to 10 percent of breast cancer patients who have localized tumors measuring over five centimeters (about two inches) in diameter. However, researchers agree that it is too early for other women to be routinely offered the option of chemotherapy before surgery.
Medications. Several exciting recent studies offer hope to millions of women that drugs to prevent and treat breast cancer are within our reach. Tamoxifen (marketed as Nolvadex) has been used for over 20 years to fend off the recurrence of breast cancer, and now it is being hailed for its potential to prevent the disease altogether. In a study of 13,000 women at high risk for breast cancer, subjects who took tamoxifen had a 45 percent lower incidence of cancer than women who received a placebo (a dummy pill). The drug was effective for women in all age groups. Although these positive results surpassed researchers' expectations, tamoxifen does pose some serious adverse effects, including an increased risk of blood clots and uterine cancer.
But hot on the heels of the tamoxifen report, more dramatic news was announced. Studies of the drug raloxifene, marketed as Evista for the treatment of osteoporosis, show that it too can reduce the incidence of breast cancer by about half without raising the risk of uterine cancer.
Tamoxifen and raloxifene are designer hormones, synthetic drugs that block the action of the female hormone estrogen, which is known to stimulate the growth of breast tumors. Since both these drugs had been previously approved by the Food and Drug Administration (FDA), doctors can legally prescribe them for any reasonable purpose (known as an off-label use). But women are being urged to wait for FDA approval of these drugs as cancer preventives. Experts are concerned about side effects, and they need to figure out who should consider taking them and who should not. Currently, another trial is slated to determine if one of these drugs is more effective than the other in preventing breast cancer.
For women who already have breast cancer, the experimental drug Herceptin represents a significant breakthrough. In one trial involving women with advanced breast cancer, Herceptin combined with chemotherapy caused cancers to disappear or shrink by half or more in 114 of 235 women. In a group that only received chemotherapy, only 74 of 234 had similar results. After one year, 78 percent of those receiving Herceptin and chemotherapy were alive compared with 67 percent in the group who received chemotherapy alone. Mild side effects included chills and fever. The usual adverse effects of standard chemotherapy, such as hair loss and decreases in blood counts, did not occur.
Herceptin trials involved women with an excess of the gene HER-2/neu in their cancerous breast cells. About 30 percent of women with breast cancer have this gene. Herceptin is a monoclonal antibody, a protein genetically engineered to bind to cancer cells and leave normal tissue alone. The drug has been granted "fast track" status by the FDA and may be approved within a year. More studies will be done to evaluate Herceptin's effects on less advanced forms of breast cancer and among ovarian cancer cases involving the same genetic defect.
What Can I Do to Protect Myself?
You can take charge of your health care by examining your breasts regularly and deciding, in consultation with your doctor, what screening course is best for you--and then sticking to it. Moreover, tell the women in your life, your mother, your sister, your daughter, to do the same.How Screening San Cave Your Life
Average size of lumps found by different screening methods: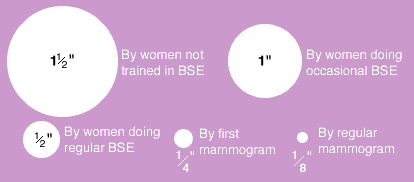
Source: Breast Health Program of New York
While mammograms are tops for finding the tiniest lumps, they aren't full-proof. That's where breast-and-life-saving measures lie in your own hands. Your self-exam could detect lumps small enough to be removed by lumpectomy.
The Debate Over Mammography
Women in their 40s are confused about whether or not to get yearly mammograms--and with good reason. For the past several years, experts have been batting different recommendations for this age group back and forth. The debate heated up again in early 1997 when an expert panel of the National Institutes of Health (NIH) said there was no evidence that mammograms save the lives of women under 50. Yet a few months after that pronouncement, the National Cancer Institute (NCI), which is affiliated with the NIH, said women in their 40s should have breast x-rays every one to two years. Why is this issue so hotly contested, and what are the latest recommendations?There's no doubt that annual mammograms for women aged 50 and older save lives. Many studies show that for these women the decrease in mortality rate is as high as 30 percent. But for younger women, several factors muddle the mammogram picture:
- Women in their forties have lower rates of breast cancer than older women do. Of 1,000 women in their forties, 16 will get breast cancer, compared with 25 out of 1,000 in the next decade of life. Scientific evidence does not show that mammograms would save these 16 lives.
- Younger women have denser breast tissue, making mammograms harder to interpret accurately. A small number of dangerous cancers (25%) in this age group will be missed by the x-ray exams.
- The younger the woman the greater the risk of getting a false positive result (detecting something that is not cancer) from a mammogram. Such results can create anxiety and often lead to unnecessary biopsies or surgeries.
- Women who get mammograms regularly are more likely to get other necessary medical care, such as Pap tests and professional manual breast exams (palpation).
- Cancer in younger women usually grows faster, making early detection all the more important.
- Certain studies show that mammograms for younger women can decrease cancer deaths (but some say this evidence is weak since the advantage does not become clear until these women are in their fifties).
Mammography Facilities: Quality Control
Until recently there was only one assurance of quality in mammography facilities: American College of Radiology (ACR) accreditation. Facilities accredited by ACR have had their equipment, personnel and procedures evaluated and approved by the college. Their doctors and other staff members are specially trained to perform and read breast x-rays. And their equipment and procedures are designed to provide high-quality mammograms with the lowest possible amount of radiation exposure.However, according to the Food and Drug Administration (FDA) only about 46 percent of all mammography facilities were accredited and many were never inspected. Concerned that not all women were receiving high quality mammography services and that breast cancer was being missed in some women, Congress passed the Mammography Quality Standards Act (MQSA) in 1992, giving the FDA the power to oversee mammography facilities. MQSA requires all mammography facilities in the United States to meet stringent quality standards, be accredited by an FDA-approved accreditation organization and be inspected annually. Quality standards include these requirements: personnel who perform mammography must be adequately trained and qualified to conduct mammography examinations and interpret results; mammography equipment must perform appropriately; and doctors and patients must be quickly and fully informed of results so that any follow-up testing or treatment can begin immediately.
According to the FDA, since MQSA was passed nearly all of the nation's 10,000 mammography facilities have been inspected and accredited. A recent Government Accounting Office report found that adherence to the new standards has had a positive effect on mammography services. Even the quality of the x-rays is up. Before MQSA, 14 percent of facilities tested were unable to pass image quality tests. Now, the nationwide figure is down to 2 percent.
Types of Surgery
Lumpectomy removes just the breast lump and usually the lymph nodes under the arm.Modified Radical Mastectomy removes the breast, the lymph nodes under the arm and the lining over the chest muscles (leaving muscles intact).
Partial or Segmental Mastectomy removes the tumor, some of the normal breast tissue around it, and some lymph nodes.
Total or Simple Mastectomy removes the tumor, some breast tissue around it and the lining of the muscle below the tumor.
For More Information
- National Cancer Institute
- Y-Me - A toll-free hotline staffed by women with breast cancer. In addition to providing information, Y-ME can direct callers who want to volunteer time or money to a breast cancer organization. 1-800-221-2141
